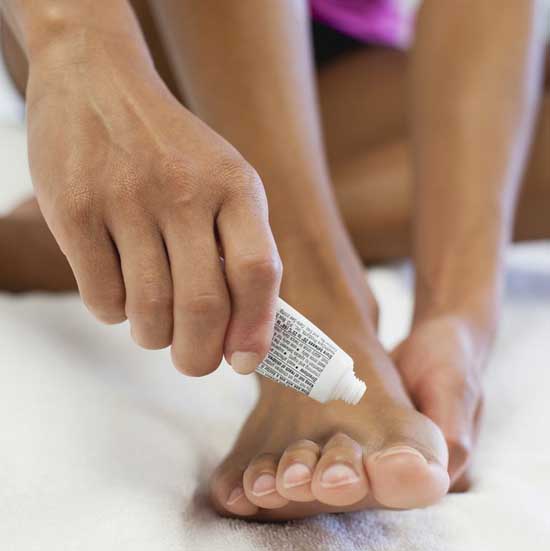
We look at the causes, symptoms and treatment of this common fungal infection.
Medically reviewed by Dr Roger Henderson and based on a text by Dr Flemming Andersen and Dr Ulla Søderberg
Suffering from itchy, cracked and scaly skin on your feet? It sounds like you might have athlete’s foot. A common condition in young people and adults, you don’t have to be a professional athlete to suffer from this fungal foot infection. Fortunately it is easily treatable.
We look at the symptoms, causes, treatments and prevention tips for athlete’s foot:
What is athlete’s foot?
Athlete’s foot, known medically as tinea pedis, is a common fungal infection that affects the feet, caused by parasites on the skin called dermatophytes.
The fungi love warm, moist places, which is why they are primarily a problem for people who wear tight-fitting trainers regularly or don’t dry their feet properly.
Athlete’s foot is contagious and it can be spread by direct skin-to-skin contact and indirectly through towels, shoes and floors etc. It can infect any part of the foot, but most often grows between the toes.
Athlete’s foot symptoms
Athlete’s foot has two variants:
• Classic athlete’s foot
The infection is caused by one of the most common fungi. Symptoms include a red itchy rash in the spaces between the toes, possibly small pustules and often a small degree of scaling. The infection can spread to the rest of the foot and other parts of the body.
• Rarer athlete’s foot
Infection of the soles of both feet by Trichophyton rubrum is a rarer variant of athete’s foot. Often the skin reddens and its furrows become marked, resembling chalked lines. If the condition is not treated, a similar rash may appear on one or both palms. After a while, the rash becomes scaly, resembling eczema.
Athlete’s foot causes
We all have one or more of the fungi that can cause athlete’s foot on our bodies. They feed on dead skin cells and are usually harmless.
Athlete’s foot is caused by parasites on the skin called dermatophytes. Dermatophytes can be divided into three groups according to their favourite hosts:
- Fungi preferring soil (geophile)
- Fungi preferring animals (zoophile)
- Fungi preferring humans (anthropophile).
Athlete’s foot is usually caused by anthropophile fungi. The most common species are Microsporum, Epidermophyton and Trichophyton. These account for 90 per cent of all skin fungal infections, commonly referred to as ringworm (tinea corporis).
The medical terms for athlete’s foot are tinea pedis or dermatophytosis palmaris, plantaris and interdigitalis – the latter indicates that, in addition to the soles and toes of the feet, the palms of the hands can also become infected.
Athlete’s foot treatment
Athlete’s foot can be treated locally with anti-fungal creams, sprays, liquids and powders that are available from your pharmacist without a prescription.
• Imidazole anti-fungals
Imidazole anti-fungals are most effective and include clotrimazole (eg Canesten AF) and miconazole (eg Daktarin).
Other antifungals include zinc undecenoate (Mycota), terbinafine (Lamisil AT) and tolnaftate (Mycil).
Treatment should be continued for two weeks after the symptoms have disappeared to ensure the infection has been treated effectively.
• Hydrocortisone anti-fungals
Some anti-fungal creams also contain hydrocortisone, eg Daktacort HC. These are useful when the skin is particularly red and inflamed, as the hydrocortisone reduces inflammation and irritation.
Hydrocortisone should not be used for longer than seven days. These anti-fungals are not suitable for children under 10-years-old or during pregnancy and breastfeeding, unless prescribed by a doctor. After seven days, treatment should be continued with a plain anti-fungal.
When to visit your GP for athlete’s foot
If the athlete’s foot has not started to respond after two weeks’ anti-fungal treatment you should see your doctor, who may prescribe a stronger anti-fungal cream or anti-fungal tablets.
The condition can sometimes disappear simply through being exposed to fresh air, but medical treatment is usually required. An infection of the foot may be accompanied by an infection of the nails.
Athlete’s foot prevention tips
There are a number of things you can do at home to minimise the chances of getting athlete’s foot:
✔️ Wash your feet daily and dry properly before putting on shoes and socks.
✔️ Use a separate towel to dry your feet.
✔️ To avoid passing the infection on you should not share towels with anyone else.
✔️ Wear socks made of cotton or wool, and change them at least twice a day or when they have become damp.
✔️ Avoid wearing shoes which are made of synthetic materials. Wear sandals or leather shoes instead.
✔️ Powder the feet and the inside of the shoes with an anti-fungal powder.
Net Doctor